Back pain is one of the most common medical complaints worldwide. Millions of people experience discomfort in the lower back, neck, or spine at some point in their lives. In many cases, the cause of this pain can be traced to problems with the spinal discs.
Two terms that are often used interchangeably are slipped disc and herniated disc. While these phrases are widely used in everyday language, they do not always mean the same thing medically. Understanding the difference between these conditions is essential for recognizing symptoms early and seeking the right treatment.
Spinal disc problems can range from mild irritation to severe nerve compression that interferes with movement and daily activities. Fortunately, many cases can be treated with conservative care, while more serious cases may require surgical intervention.
In this comprehensive guide, we will explore:
• What spinal discs are and how they function
• The difference between a slipped disc and a herniated disc
• Common symptoms of disc-related spine conditions
• Causes and risk factors
• Diagnosis and imaging tests
• Non-surgical treatment options
• When surgery may be necessary
• Recovery and prevention strategies
Understanding these conditions can help patients make informed decisions about their spine health and seek timely medical care when needed.
Understanding the Role of Spinal Discs
The spine is made up of a series of bones called vertebrae. Between each vertebra sits a soft, cushion-like structure known as an intervertebral disc.
Spinal discs serve several important functions:
• acting as shock absorbers for the spine
• allowing flexibility and movement
• preventing vertebrae from rubbing against each other
• distributing pressure across the spine
Each disc has two main components:
Outer layer (annulus fibrosus)
A tough outer ring that protects the disc.
Inner gel-like center (nucleus pulposus)
A soft, jelly-like core that absorbs pressure and movement.
When the structure of the disc becomes damaged or weakened, it can bulge or rupture. This can place pressure on nearby spinal nerves and lead to significant pain.
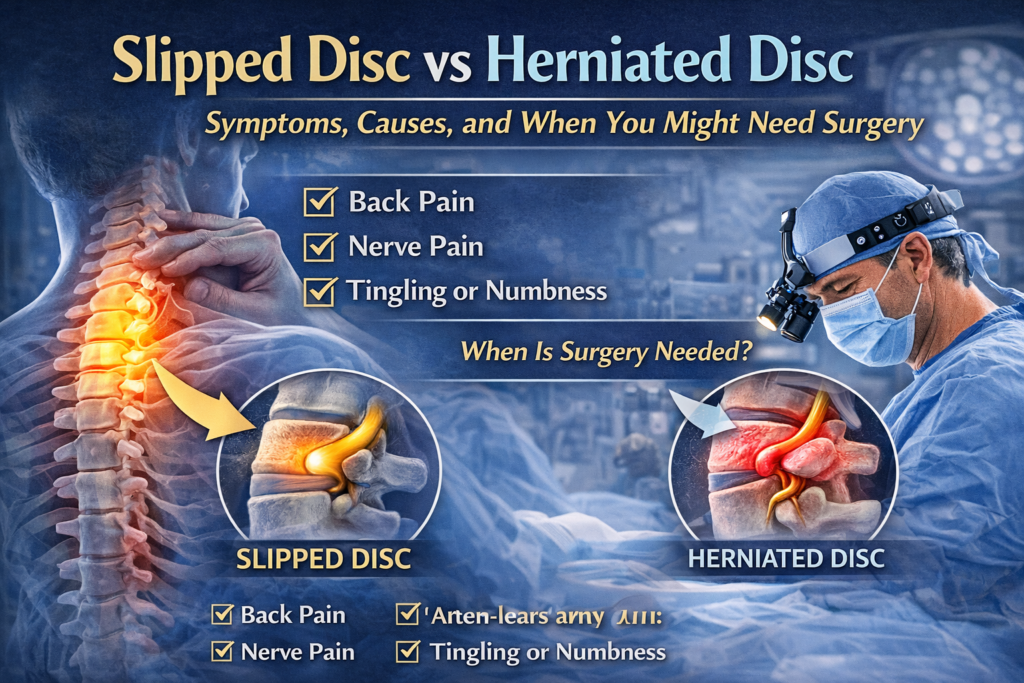
Slipped Disc vs Herniated Disc: What Is the Difference?
The terms slipped disc and herniated disc are often used interchangeably, but medically they describe slightly different conditions.
| Condition | Description | Common Symptoms |
|---|---|---|
| Slipped Disc | Disc shifts or bulges out of its normal position | Back pain, stiffness |
| Herniated Disc | Inner disc material pushes through the outer layer | Nerve pain, numbness, weakness |
The phrase slipped disc is commonly used in everyday language, but discs do not actually slip out of place. Instead, the disc bulges or protrudes.
A herniated disc occurs when the outer layer of the disc tears and the inner material leaks outward. This can place pressure on nearby nerves, leading to more severe symptoms.
Where Do Disc Problems Most Often Occur?
Disc problems most commonly occur in two areas of the spine.
Lumbar Spine (Lower Back)
The lumbar spine supports most of the body’s weight, making it more vulnerable to disc injuries.
Symptoms may include:
• lower back pain
• pain radiating down the leg (sciatica)
• numbness in the feet or legs
Cervical Spine (Neck)
Disc problems can also occur in the cervical spine.
Symptoms may include:
• neck pain
• shoulder pain
• numbness in the arms or hands
• tingling in the fingers
Disc issues in this region may also cause headaches.
Common Symptoms of a Herniated or Slipped Disc
Symptoms vary depending on the location and severity of the disc problem.
Common symptoms include:
• persistent back pain
• sharp pain in the neck or spine
• numbness or tingling in arms or legs
• muscle weakness
• burning nerve pain
• reduced mobility
In severe cases, nerve compression may cause difficulty walking or performing everyday activities.
Causes of Disc Injuries
Disc problems can develop gradually over time or occur suddenly due to injury.
Some of the most common causes include:
Age-Related Degeneration
As people age, spinal discs gradually lose water content and elasticity.
This makes them more prone to:
• tearing
• bulging
• herniation
Heavy Lifting
Improper lifting techniques place excessive pressure on the spine.
This can cause discs to rupture or bulge.
Poor Posture
Prolonged sitting, slouching, or poor ergonomic habits can stress spinal discs over time.
Sports Injuries
High-impact sports or sudden twisting movements may cause disc damage.
Accidents or Trauma
Car accidents or falls can place significant force on the spine.
Risk Factors for Disc Problems
Certain lifestyle and health factors increase the risk of developing spinal disc conditions.
These include:
• obesity
• smoking
• sedentary lifestyle
• repetitive physical strain
• genetics
• physically demanding occupations
Addressing these risk factors can help reduce the likelihood of disc injuries.
How Doctors Diagnose Disc Problems
Accurate diagnosis is essential for determining the best treatment plan.
Doctors may use several diagnostic tools.
Medical History and Physical Examination
A doctor will first review symptoms and perform a neurological exam.
This may include testing:
• reflexes
• muscle strength
• sensation
• coordination
Imaging Tests
Imaging helps confirm the diagnosis.
Common imaging tools include:
• MRI scans
• CT scans
• spinal X-rays
MRI scans are especially useful for identifying disc herniation and nerve compression.
Non-Surgical Treatments for Herniated Discs
The good news is that most herniated disc cases improve without surgery.
Doctors usually recommend conservative treatments first.
Physical Therapy
Physical therapy helps strengthen the muscles that support the spine.
Exercises may include:
• core strengthening
• stretching
• posture training
Medications
Doctors may prescribe medications to reduce pain and inflammation.
Examples include:
• anti-inflammatory medications
• muscle relaxants
• nerve pain medications
Epidural Steroid Injections
Steroid injections reduce inflammation around spinal nerves and provide pain relief.
These injections are commonly used for:
• sciatica
• herniated discs
• spinal stenosis
Lifestyle Modifications
Simple lifestyle adjustments can greatly improve spinal health.
These include:
• improving posture
• maintaining healthy body weight
• regular exercise
• ergonomic work environments
When Surgery May Be Necessary
While many patients recover without surgery, certain situations require surgical treatment.
Surgery may be recommended if:
• severe nerve compression exists
• muscle weakness worsens
• symptoms persist after months of treatment
• spinal instability occurs
• loss of bladder or bowel control develops
These symptoms may indicate serious nerve damage.
Common Surgical Procedures for Herniated Discs
Several surgical options may be used to treat disc problems.
| Procedure | Purpose |
|---|---|
| Microdiscectomy | Removes the damaged portion of the disc |
| Laminectomy | Relieves pressure on spinal nerves |
| Spinal Fusion | Stabilizes the spine |
| Artificial Disc Replacement | Replaces a damaged disc |
Many procedures are now performed using minimally invasive techniques.
Minimally Invasive Spine Surgery
Modern spine surgery has advanced significantly in recent years.
Minimally invasive procedures use small incisions and specialized instruments.
Benefits include:
• less tissue damage
• faster recovery
• shorter hospital stays
• reduced pain after surgery
These techniques have improved outcomes for many patients with disc problems.
Recovery After Disc Surgery
Recovery time depends on the procedure and overall health of the patient.
Typical recovery milestones may include:
• walking within days after surgery
• gradual return to work within weeks
• full recovery within several months
Physical therapy is often recommended to restore strength and mobility.
Preventing Future Disc Problems
Taking care of your spine can help prevent future injuries.
Healthy habits include:
• maintaining good posture
• exercising regularly
• strengthening core muscles
• avoiding heavy lifting injuries
• staying active throughout the day
Preventive care plays an important role in long-term spine health.
Frequently Asked Questions
Is a slipped disc the same as a herniated disc?
Not exactly. A slipped disc usually refers to a bulging disc, while a herniated disc occurs when the inner material pushes through the outer layer.
Can a herniated disc heal without surgery?
Yes. Many cases improve with conservative treatments such as physical therapy and medications.
How long does it take to recover from a herniated disc?
Recovery varies, but many patients improve within a few weeks to several months.
Is herniated disc surgery safe?
Modern surgical techniques are highly effective and often performed using minimally invasive methods.
Final Thoughts
Spinal disc problems can significantly affect quality of life, causing pain, numbness, and mobility issues. Understanding the difference between slipped discs and herniated discs can help patients recognize symptoms early and seek appropriate treatment.
Fortunately, most disc problems can be managed without surgery. However, when symptoms become severe or nerve damage develops, surgical treatment may offer lasting relief.
If you are experiencing persistent back pain, nerve pain, or weakness in your arms or legs, consulting a qualified neurosurgeon can help identify the cause and determine the best treatment approach.
Early diagnosis and proper care can protect your spine health and help you return to an active, pain-free life.

